 In the United States, one in eight women will develop breast cancer at some point in their lives. At 12 percent of the adult female population, this means that aside from nonmelanoma skin cancer, breast cancer is the most commonly diagnosed cancer in women. Breast cancer causes the most cancer-related deaths in women, second to lung cancer. Potentially, 41,760 women will die from breast cancer in 2019.
In the United States, one in eight women will develop breast cancer at some point in their lives. At 12 percent of the adult female population, this means that aside from nonmelanoma skin cancer, breast cancer is the most commonly diagnosed cancer in women. Breast cancer causes the most cancer-related deaths in women, second to lung cancer. Potentially, 41,760 women will die from breast cancer in 2019.
There is hope. Better diagnostic tools, treatment protocols, and even regular self-exam routines can make a big difference. You can potentially prevent breast cancer through education and good health practices.
A Quick Overview of Breast Cancer
It’s important to know what breast cancer does in the body. The breasts are composed of three different types of tissue: lobules, ducts, and connective tissue. Lobules produce milk, ducts transport that milk to the nipple, and connective tissue surrounds and holds together all the breast tissue.
In cancer, cells in these tissues — usually in either the lobules or the ducts — begin to grow uncontrollably. This creates a tumor, and in some cases these out-of-control cells can spread (metastasize) to other parts of the body through the lymphatic system and blood vessels and cause harm. At this point, it’s crucial to seek treatment from a breast care center.
How Common is Breast Cancer? Five Facts You Need to Know
 When it comes to staying proactive about breast cancer, education is the first step. It’s important to know the risks factors so that you can stay on top of your health.
When it comes to staying proactive about breast cancer, education is the first step. It’s important to know the risks factors so that you can stay on top of your health.
#1: Breast Cancer Becomes More Common With Age
According to the most recent SEER (Surveillance, Epidemiology, and End Results Program) results from the National Cancer Institute, this is how a woman’s breast cancer risk changes by decade:
- Age 30 – 1 in 227
- Age 40 – 1 in 68
- Age 50 – 1 in 42
- Age 60 – 1 in 28
- Age 70 – 1 in 26
It’s important to receive check-ups such as mammograms with your doctor at regular intervals to keep up with any changes in breast tissue.
#2: Breast Cancer is More Common with Certain Genetic Factors
Chances are, you know someone who has developed breast cancer. In fact, 3.1 million women in the U.S. alone have a history of breast cancer. If a close family member has been diagnosed with breast cancer, it’s important to be aware of your genetic risk factors.
For example, your chance of getting breast cancer nearly doubles if you have a sister, daughter, or mother who has been diagnosed. According to the latest research, mutations in certain genes — like the BRCA1 and BRCA2 genes — can increase your chances significantly. Women with the BRCA1 gene have around a 72percent chance of developing cancer, while those with the BRCA2 gene have a 69percent lifetime risk.
Though around 5-10 percent of women with breast cancer have inherited genes that make them more likely to get cancer, 85 percent of women who develop it have no family history. This means that, even if you don’t have a family history, it’s important to seek regular preventative treatment.
#3: Breast Cancer Affects Men, Too
Though it is significantly more common in women, breast cancer can affect men as well. Men, too, have breast cancer skin and tissue that is vulnerable to cancer, but at a significantly lower rate. In fact, only one in 1,000 men will be diagnosed with breast cancer. Unfortunately, there is a higher fatality rate for men with breast cancer — most likely because they are not as aware of the risks, and may not seek diagnosis and treatment quickly enough.
#4: Certain Lifestyle Factors Increase Risk
Although it’s possible to be diagnosed with breast cancer without any of the associated risk factors, it’s important to know what sorts of lifestyle practices can put you at a greater statistical risk for breast cancer:
- Alcohol use. For women who regularly have two or three drinks per day, there is a 20% higher risk of getting breast cancer.
- Obesity. If you are overweight or obese after menopause, you may be at a greater risk of developing breast cancer.
- Lack of physical activity. For women past menopause, lack of physical activity is considered a risk factor. According to the American Cancer Society, it’s important to get 150 minutes of moderate activity or 75 minutes of intense activity every week.
- Birth control use. Certain hormonal birth control methods — like oral contraceptives, the birth control shot, and birth control implants — can slightly increase the risk of breast cancer.
- Childbirth/Breastfeeding factors. In some cases, having a child before the age of 30 has been shown to decrease the risk of certain types of cancer. Also, breastfeeding for 1.5 to 2 years can decrease the risk of breast cancer.
- Hormone therapy. Some women get hormone therapy during menopause to help prevent osteoporosis and lessen menopause symptoms. This is linked in some cases to higher rates of breast cancer. Can you please provide a source to back this claim? I thought this has been proven wrong in recent years because of way less estrogen is used in current hormone therapy?
#5: Breast Cancer is as Common as Ever — But Survival Rates are Increasing
In recent years, the rates of breast cancer have increased by a very small amount: 0.4% per year. However, despite slightly increased incidence rates, mortality rates have decreased drastically. In 1985, breast cancer death rates reached their highest — 32.98 deaths per 100,000 women in the U.S. From 1989 to 2016 (the most recent data available) death rates have decreased by 40 percent in women over 50. For younger women, death rates have remained relatively steady since 2007.
It’s thought that the spread of awareness and education about breast cancer — coupled with more effective treatments — has contributed to the overall increasing rates of survival.
What You Can Do: Self-Exams, Clinical Exams, and Mammograms
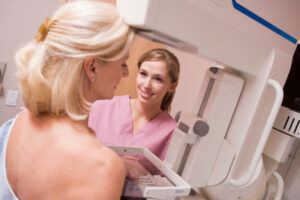 When it comes to breast cancer, early detection makes a significant difference. There are several steps you can take to detect breast changes, and also some breast care services you should seek to stay proactive.
When it comes to breast cancer, early detection makes a significant difference. There are several steps you can take to detect breast changes, and also some breast care services you should seek to stay proactive.
- Know signs & symptoms. Though not everyone who gets breast cancer experiences any signs or symptoms, it’s important to follow-up with any changes in nipple discharge, breast pain or sensation, or changes in the texture or appearance of breasts.
- Self-exams. It’s extremely important to perform a monthly breast self-exam. In fact, for 40 percent of cancers that are diagnosed, treatment was sought because a woman felt a lump during a self-exam.
- Clinical breast exam. Though it’s important to do a monthly exam at home, it’s also pivotal to get an annual clinical breast exam from a health professional. A doctor or nurse might notice something that went undetected during a home exam.
- Mammogram. With a specialized x-ray called a mammogram, your breast health team can detect abnormalities in breast tissue. The National Breast Cancer Foundation recommends that women who are 40 or older should have mammograms every one or two years. For younger women, you should talk to your doctor about any genetic or lifestyle factors to come up with a personalized mammogram plan.
A Professional Breast Care Center Can Make All the Difference
It’s estimated that 268,800 new cases of invasive breast cancer will be diagnosed in 2019. To help prevent cancer, it’s important to stay proactive about your health and lifestyle, track any breast changes, and do regular self-breast exams. In addition, partnering with a breast health team can make all the difference. At Weiss Memorial Hospital in Chicago, the compassionate team at the Breast Care Center can help detect, diagnose, and treat breast cancer. If you would like to learn more or make an appointment, please contact us today.

